Locating cell origin provides foundation for brain injury cure Thursday, 24 July 2008 Adult stem cells originate in a different part of the brain than is commonly believed, and with proper stimulation they can produce new brain cells to replace those lost to disease or injury, a study by UC Irvine scientists has shown. Evidence strongly shows that the true stem cells in the mammalian brain are the ependymal cells that line the ventricles in the brain and spinal cord, rather than cells in the subventricular zone as biologists previously believed. Brain ventricles are hollow chambers filled with fluid that supports brain tissue, and a layer of ependymal cells lines these ventricles. Knowing the cell source is crucial when developing stem cell-based therapies. Additionally, knowing that these normally dormant cells can be coaxed into dividing lays the groundwork for future therapies in which a patient's own stem cells produce new brain cells to treat neurological disorders and injuries such as Parkinson's disease, stroke or traumatic brain injury. "With such a therapy, we would know which cells in the body to target for activation, and their offspring would have all the properties necessary to replace damaged or missing cells," said Darius Gleason, lead author of the study and a graduate student in the Department of Developmental and Cell Biology, the UCI Sue and Bill Gross Stem Cell Research Center. "It is a very promising approach to stem cell therapy." Study results appear this month online in the journal Neuroscience. Stem cells are the "master cells" that produce each of the specialized cells within the human body. If researchers could control the production and differentiation of stem cells, they may be able to use them to replace damaged tissues. One focus of stem cell research is transplantation, which entails injecting into the body healthy cells that may or may not genetically match the patient. Transplantation of non-matching stem cells requires the use of drugs to prevent the body from rejecting the treatment. But, working with a patient's own cells would eliminate the need for transplantation and immunosuppressant drugs and may be a better alternative, scientists say. Ependymal cells line the fluid-filled ventricles, so a drug to activate the cells could theoretically travel through this fluid directly to the stem cells. "The cells already match your brain completely since they have the same genetic make-up. That is a huge advantage over any other approach that uses cells from a donor," Gleason said. "If they are your cells, then all we are doing is helping your body fix itself. We're not reinventing the repair process." In this study, Gleason and Peter Bryant, developmental and cell biology professor, used rats treated to develop the animal equivalent of Parkinson's disease. They chose this type of rat because in a previous study by UCI collaborator James Fallon, a small protein given to the brain-damaged rats sparked a rapid and massive production and migration of new cells, and significantly improved motor behavior.
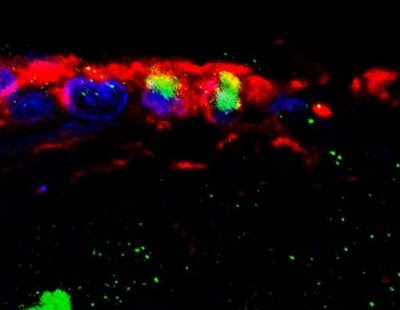
First, the UCI researchers sought to determine the true location of stem cells in the rats by looking for polarized cells, which have different sets of proteins on opposite sides so that when one divides it can produce two different products. Polarization gives rise to asymmetric cell division, which produces one copy of the parent and a second cell that is programmed to turn into another cell type. Asymmetric cell division is the defining characteristic of a stem cell. On rat brain samples, the researchers applied antibodies to identify proteins that may be involved in asymmetric cell division, and they found that polarization exists on the ependymal cells. "It couldn't have been a stronger signal or clearer message. We could see that the only cells undergoing asymmetric cell division were the ependymal cells," Gleason said. Next, they gave a drug to induce cell division in the rats and examined their brains at intervals ranging from one to 28 days after the treatment. At each interval, they counted cells that were dividing in the ependymal layer. They found the most division at 28 days, when about one-quarter of the ependymal cells were dividing. Previous studies by researchers at other institutions were successful in getting only a few cells to divide in that layer. "One interpretation of previous studies is there are scattered stem cells in the ependymal layer, and it is hard to locate them," Bryant said. "But we believe that all of the ependymal cells are stem cells, and that they all have the ability to be activated." Researchers don't know yet what sparks cell division at the molecular level, but learning that process and how to control it could lead to a safe, effective stem cell therapy. About the University of California, Irvine: The University of California, Irvine is a top-ranked university dedicated to research, scholarship and community service. Founded in 1965, UCI is among the fastest-growing University of California campuses, with more than 27,000 undergraduate and graduate students and nearly 2,000 faculty members. The third-largest employer in dynamic Orange County, UCI contributes an annual economic impact of $3.6 billion. See also: Adult Stem Cells Reprogrammed in the Brain CellNEWS - Monday, 30 June 2008 ......... ZenMaster
For more on stem cells and cloning, go to CellNEWS at http://cellnews-blog.blogspot.com/ and http://www.geocities.com/giantfideli/index.html





No comments:
Post a Comment